Pediatric Otolaryngology

Although children are often affected by the same ear, nose and throat conditions as adults, they often require special care to treat these complex conditions. Children are often more susceptible to ENT conditions and are commonly affected by chronic ear infections, tonsillitis, congenital defects, voice and speech disorders, sleep apnea and more. Our doctors are specially trained to diagnose and treat the unique conditions that affect children. We strive to provide the most effective treatment while taking into consideration the comfort of our patients and concerns of their parents.
Airway Reconstruction
Obstructions within the airway, which may occur in the trachea, voice box (larynx) or throat (pharynx) are often serious conditions that can lead to difficulty breathing, choking, difficulty swallowing, wheezing and other troubling symptoms. These blockages may develop as a result of an allergic reaction, infection, trauma, foreign body, cancer or other diseases that prevent air from flowing normally through the passage.
In order to relieve these symptoms and restore proper breathing, surgical treatment in the form of airway reconstruction may be needed. There are several different procedures that may be performed to correct these blockages, including tracheoscopy, laryngoscopy, bronchoscopy, tracheotomy, laryngotracheoplasty and others.
These procedures are performed to correct breathing difficulties caused by a congenital defect or previous medical procedure, as well as:
- Tracheal or laryngeal deformities
- Abnormalities caused by intubation
- Tracheal stenosis, subglottic stenosis, laryngeal cleft and laryngeal atresia
- Abnormalities caused by tracheotomy tube removal
Airway reconstruction procedures may be performed using open or endoscopic techniques, depending on the type of procedure being performed and the severity of the child's condition. Open procedures involve making an incision in the neck to access the airway, while endoscopic procedures are performed through the mouth and do not require any incision.
Otology
Otology involves the diagnosis and treatment of ear diseases, including tinnitus, ear infections (otitis media), and congenital cholesteatomas, congenital sensorineural hearing loss, congenital syndromes, and others. These conditions may cause symptoms such as ear pain, headaches, fever, dizziness, hearing loss and discharge. Many ear conditions are especially common in children, who may require special care for their condition.
Treatment for these conditions often involves hearing aids, ear tubes, medication, surgery or other approaches. Your doctor will decide which treatment is best for you after a thorough evaluation of your condition and overall health.
Ear Infections
Ear infections are one of the most common diseases in children and occur most often between the ages of four months and five years. An infection occurs when excess fluid, often as a result of a cold, becomes trapped in the eustachian tubes or infected by bacteria. This fluid pushes against the eardrum and causes pain.
Aside from pain, ear infections can also cause:
- Hearing loss
- Fever
- Irritability
- Discharge from the ear canal
- Difficulty sleeping
We treat these either with antibiotics or procedures such as tympanostomy tubes for recurrent or chronic otitis media.
Tonsillitis/Adenoiditis
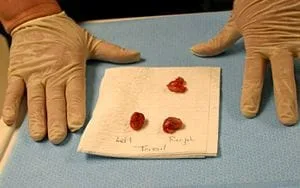
Tonsillitis is an inflammation of the tonsils, caused by a virus or bacteria. This condition is common in children and spreads through contact with throat or nasal fluids. The tonsils become swollen, red and painful and may be coated with a yellow or white substance.
Most cases of tonsillitis are caused by a virus, although it can sometimes be caused by the same bacteria that causes strep throat. Tonsillitis symptoms include:
- Sore throat
- Difficulty swallowing
- Fever
- Swollen lymph nodes
Your doctor will usually be able to identify tonsillitis by finding red and swollen tonsils with spots or sores on them. A rapid strep throat test may also be performed to determine the cause. Tonsillitis can usually be treated at home through rest and drinking plenty of liquids. Antibiotics may be prescribed for bacterial infections. Surgery to remove the tonsils may be recommended if a child has recurrent throat infections or a one persistent infection.
For more information on Pediatric ENT, please visit
- http://www.entnet.org/HealthInformation/pediatric.cfm
Also check out our informative sheet on
Tonsils and Adenoids

Neck Masses
A neck mass is a common childhood condition that involves swelling that changes the shape of the neck. Neck masses do not usually cause any symptoms and often disappear on their own, although they should be evaluated by your child’s doctor to determine if treatment is necessary.
There are several different types of common neck masses, including:
- Branchial Cleft Cyst – formation of tissue that forms on the neck during embryonic development after failure to develop normally
- Reactive Lymph Nodes – enlarged lymph nodes that develop as a reaction to an infection or autoimmune condition
- Lymphoma – cancerous mass that develops in the lymph nodes due to DNA damage or changes
- Thyroglossal duct cyst – develops from the cells and tissues that remain after the thyroid gland forms during embryonic development
Neck masses that last more than a few weeks should undergo diagnostic testing. Depending on the type, size and location of the mass, your child’s doctor may perform an imaging exam such as an ultrasound, CT scan or MRI for a magnified view of the mass, or a biopsy to test for any cancerous cells.
Treatment for a pediatric neck mass can vary depending on each individual lesion, but may include regular observation to detect any growth or abnormalities, antibiotics for infected masses or resection to surgically remove the mass and reduce the risk of cancer or other complications.
